Medicine and Health
Advancements in nanoparticle-based treatment approaches for skin cancer therapy
L. Zeng, B. H. J. Gowda, et al.
Skin carcinoma, comprising melanoma and non-melanoma types (basal cell carcinoma and squamous cell carcinoma), is highly prevalent globally, with significant morbidity and mortality—particularly from melanoma, which accounts for ~80% of skin cancer deaths. Risk factors include ultraviolet radiation, chemical carcinogens, genetic factors, fair skin, and immunosuppression. Standard treatments (excision/Mohs surgery, radiotherapy, curettage and electrodesiccation, cryotherapy, photodynamic therapy, and in advanced stages chemotherapy, targeted therapy, and immunotherapy) face limitations including recurrence risk, high cost, systemic toxicity, poor bioavailability, limited tumor targeting, and patient noncompliance. Five-year survival for advanced melanoma remains suboptimal (regional nodes 68%, distant metastasis 30%). Nanotechnology offers a potential solution: nanoparticles can function as therapeutic agents and carriers, enabling passive/active tumor targeting, overcoming drug resistance, enhancing stability and solubility, controlling release, and improving cutaneous delivery by enhancing skin permeability. Several nanoformulations have FDA/EMA approvals in other cancers, underscoring translational promise. This review summarizes skin cancer types/pathology, current treatments and limitations, and provides an up-to-date synthesis of inorganic, polymer-based, and lipid-based nanoparticles in skin cancer therapy, including patents and clinical trials, highlighting their advantages and challenges.
Types and pathology: Basal cell carcinoma (accounts for ~70% of cutaneous malignancies) arises from basal epidermal cells; subtypes include nodular, superficial, micronodular, and infiltrative, with ultraviolet-B-induced mutations (e.g., p53, Ras, hedgehog pathway). Squamous cell carcinoma (~25% of cutaneous malignancies) is more invasive than BCC; risk factors include UV exposure, HPV, chemical carcinogens, and inflammatory conditions, with potential for metastasis. Melanoma (~5% of cases) is most lethal, originating from melanocytes, progressing from radial growth in the epidermis to vertical invasion and metastasis; staging (0–IV) correlates with thickness, ulceration, nodal involvement, and distant spread.
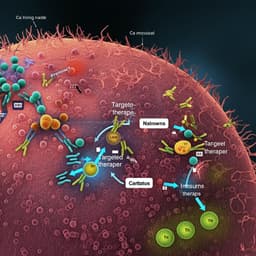
Current treatments and limitations: Early-stage disease is managed with excision/Mohs surgery, radiation therapy, curettage/electrodesiccation, cryotherapy, laser, and photodynamic therapy; adjuvant targeted and immune therapies reduce recurrence. Advanced/metastatic disease relies on systemic immunotherapy, targeted therapy, and chemotherapy. Limitations include high cost and access issues (immunotherapy/targeted therapy), systemic toxicity, chemoresistance, poor tumor targeting, low bioavailability, and inadequate penetration of agents in topical settings due to the stratum corneum.
Rationale for nanotechnology: Nanoparticles (1–1000 nm) enable enhanced permeability and retention (EPR)-mediated passive targeting and can be engineered for active targeting, prolonged circulation (RES evasion), controlled release, and improved topical/transdermal delivery. Evidence across inorganic (e.g., mesoporous silica, gold, silver, zinc oxide, carbon nanotubes, cerium oxide, platinum, copper), polymer-based (micelles, dendrimers, PLGA and other polymeric nanoparticles), and lipid-based platforms (SLNs, NLCs, liposomes, niosomes, transferosomes, ethosomes) demonstrates improved antitumor efficacy, reduced systemic toxicity, and synergy with photothermal/photodynamic and immunotherapies. The review compiles preclinical studies (in vitro/in vivo), discusses mechanisms (e.g., ROS generation, ferroptosis, apoptosis, immune modulation), delivery routes (intravenous, intratumoral, topical, microneedles), and translational aspects including patents and clinical trials.
- Nanoparticles as dual-function platforms: Many inorganic nanoparticles (e.g., ZnO, Ag, Au, CNTs, CeO2, Pt, Cu) exhibit intrinsic anticancer properties (e.g., ROS generation, mitochondrial dysfunction, ferroptosis induction) while also serving as drug carriers and photothermal/photosensitizing agents for combined therapies (chemo-PTT/PDT).
- Mesoporous silica nanoparticles (MSNs): Enable high loading and controlled release; examples include cisplatin@SBA-15 improving in vivo tumor inhibition with reduced toxicity; cancer cell membrane-coated DTIC@MSNs enhanced tumor accumulation and, combined with anti-PD-1, doubled in vitro cell death vs. free DTIC; siRNA-loaded MSNs with PLL coating achieved superior topical delivery and tumor inhibition compared with intratumoral/intravenous routes.
- Carbon nanotubes: Demonstrated intrinsic antimelanoma activity via caspase-3 activation and interference with cytoskeletal division; targeted and combination regimens (e.g., RGDK-SWCNTs for curcumin delivery; CpG and doxorubicin on MWCNTs plus NIR) enhanced tumor ablation.
- Metal/metal-oxide NPs: ZnO NPs showed size-dependent cytotoxicity and synergy as PDT/PTT agents; Ag@ZnO enhanced ROS and selectively killed melanoma cells upon UV; RNA corona (poly I:C) on ZnO yielded synergistic anti-melanoma effects in vitro and in vivo; Au core–silica–ZnO QD gatekeepers allowed pH-responsive DOX release plus PTT, achieving maximal tumor inhibition with NIR.
- Gold nanoparticles: Gum arabic-coated Au nanorods reduced normal cell toxicity and inhibited melanoma growth; Sorafenib-derivative capped AuNPs improved oral efficacy; immune cell hitchhiking with bacteria-mimetic AuNPs enhanced PTT/immunotherapy; miR-21-3p–AuNPs sensitized tumors to anti-PD-1 via ferroptosis.
- Silver nanoparticles: Biogenic and stabilized AgNPs exhibited selective melanoma cytotoxicity and synergized with DOX or anti-PD-1; size and capping agents modulated uptake and selectivity; combination with ICG enabled effective PTT.
- Dendrimers and polymeric micelles/NPs: PAMAM dendrimers improved topical vismodegib delivery for BCC and enabled targeted DOX release (cRGD-PAMAM); micelles facilitated topical paclitaxel and siRNA delivery with enhanced skin penetration and efficacy; PLGA-based targeted, reduction-responsive systems (cRGD-sPLGA) outperformed Lipo-DOX (IC50 0.92 µg/mL, 12.3× lower than Lipo-DOX) with superior tumor accumulation.
- Lipid-based carriers: SLNs and NLCs improved oral/topical delivery of chemotherapeutics (e.g., DHA-dFdC, docetaxel, paclitaxel) and phytoconstituents (curcumin/resveratrol, quercetin), achieving higher bioavailability, skin deposition, and tumor inhibition with reduced toxicity; transferosomes/ethosomes enhanced penetration of large/hydrophilic agents like Rose Bengal and vismodegib; combinatorial liposomal vaccines (peptide + IDO inhibitor) amplified antitumor immunity.
- Microneedle (MN) platforms: Dissolving and hollow MNs enabled localized, repeated, and spatiotemporally controlled release (e.g., PTX/IR-780 SLNs achieving 100% tumor eradication in 30 days in vivo with NIR-triggered pulses); MNs improved delivery of siRNAs (BRAF, STAT3) and PDT agents (hypericin).
- Translation: The review catalogs recent patents and clinical trials leveraging nano-based therapeutics (many repurposing approved nanoformulations) for melanoma and non-melanoma skin cancers, highlighting growing clinical interest though no nano-therapeutic is yet approved specifically for skin cancer.
The review consolidates evidence that nanoparticle platforms address central limitations of current skin cancer treatments by improving tumor selectivity and accumulation (via EPR and active targeting), enhancing drug solubility/stability, enabling controlled and stimuli-responsive release, and reducing systemic exposure and toxicity. In topical applications, nanoformulations and MNs overcome the stratum corneum barrier, allowing localized, high-concentration delivery to cutaneous tumors. Inorganic nanoparticles provide multimodal therapy by combining intrinsic ROS-mediated cytotoxicity or photothermal/photosensitizing effects with drug delivery, leading to synergistic antitumor responses and potential immune activation (e.g., ICD, ferroptosis sensitizing to checkpoint blockade). Polymeric and lipid-based systems expand the therapeutic repertoire to include siRNA/miRNA, immunomodulators, and combinations, increasing efficacy while lowering doses and side effects. Collectively, these findings support the hypothesis that nanotechnology can refine and potentiate immunotherapy, targeted therapy, and chemotherapy for skin cancers and enable minimally invasive local treatments for early lesions.
Nanoparticle-based strategies—spanning inorganic, polymeric, and lipid platforms—significantly enhance the therapeutic index of skin cancer treatments by enabling targeted, multimodal, and controllable delivery with reduced systemic toxicity. They improve outcomes across routes (intravenous, intratumoral, oral, topical, and microneedle-mediated) and synergize with photothermal/photodynamic and immunotherapies. Despite promising preclinical data, translation remains limited: no nano-therapeutic is yet approved specifically for skin cancers. Future research should prioritize: rigorous safety, pharmacokinetics, and biodistribution studies; scalable, reproducible manufacturing; optimization of targeting and stimuli-responsiveness; integration with immune checkpoint and vaccine strategies; and well-designed clinical trials, particularly for topical/MN-based localized therapies and combination regimens.
- Predominantly preclinical evidence: Many studies are in vitro or in small animal models; human clinical data for skin cancer nano-therapies are limited.
- EPR variability and limited passive targeting: Tumor accumulation via EPR is inconsistent; passive targeting often delivers <1% of injected dose to tumors.
- Safety and toxicity: Long-term biocompatibility, RES interactions, and off-target effects—especially for inorganic NPs—require further evaluation; cationic components and surfactants can add toxicity.
- Skin delivery barriers: While nanoformulations and MNs enhance penetration, efficacy depends on formulation properties, application methods, and lesion depth; standardization is needed.
- Manufacturing and scalability: Complex surface functionalization and biomimetic coatings may pose challenges for reproducibility and GMP scale-up.
- Cost and access: Some advanced nano-immuno/phototherapies may remain costly without optimization.
- Lack of approved nanoformulations specifically for skin cancer: Despite numerous patents and trials, no dedicated nano-based skin cancer therapy is yet commercialized.
Related Publications
Explore these studies to deepen your understanding of the subject.