Medicine and Health
Therapeutic B-cell depletion reverses progression of Alzheimer’s disease
K. Kim, X. Wang, et al.
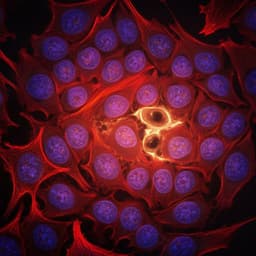
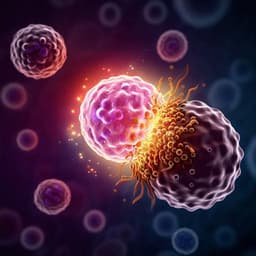
This groundbreaking research explores the crucial role of B cells in Alzheimer's disease (AD), revealing their accumulation and infiltration in the brain, and suggesting that targeting these cells may provide a promising therapeutic strategy for AD patients. Conducted by leading experts including Ki Kim, Xin Wang, and others from the National Institute on Aging, this study highlights the potential for B cell depletion to reshape the future of AD treatment.
Related Publications
Explore these studies to deepen your understanding of the subject.